Our scientific profile
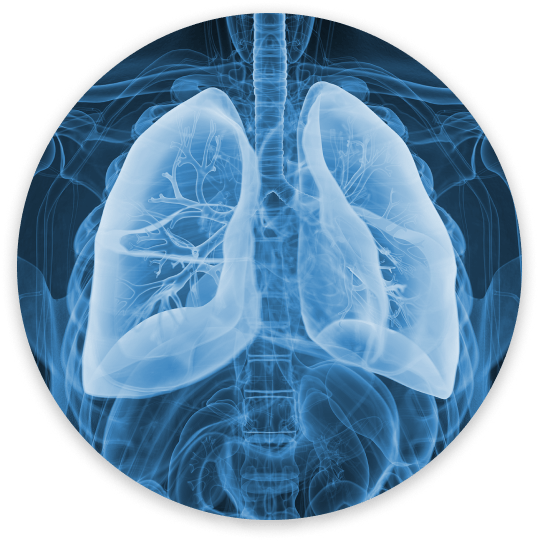
Our research focuses on investigating acute lower respiratory tract infections and their impact on public health. There is an urgent medical need for new and effective therapeutic approaches for lung infections, particularly for ARDS (Acute Respiratory Distress Syndrome) and ALI (Acute Lung Injury), which have a high mortality rate.
Viral infections are the primary cause of CAP (Community-Acquired Pneumonia) and ARDS, highlighting the necessity for a better understanding of the underlying pathobiology.
Acute lower respiratory tract infections represent an increasing public health problem worldwide, and result in a disease burden greater than that of any other infection, with mortality rates unchanged over the past 50 years. Likewise, the lack of any pharmacological treatments for the most devastating clinical course of pulmonary infection, acute lung injury (ALI) or acute respiratory distress syndrome (ARDS), underscores an urgent medical need for novel, effective therapeutic approaches.
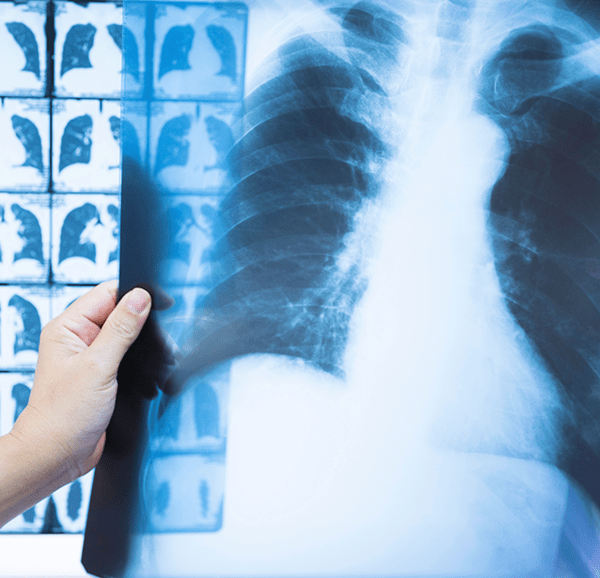

Genetic susceptibilities together with specific pre-conditions or co-morbidities are major risk factors for severe courses of respiratory viral disease, characterized by deficiencies in adequate antiviral control and/or exaggerated inflammation and tissue damage. In addition, there is increasing evidence that respiratory virus infection frequently predisposes for severe gram-positive bacterial superinfections with fatal outcome. In general, resolution of pulmonary inflammatory processes due to infectious (i.e. viral) or non-infectious (i.e. acid aspiration) causes increase the susceptibility for bacterial infections.

Against this background, our research is dedicated to unraveling the mechanisms driving anti-viral host defense, to dissecting the cellular and molecular contributors to the tissue damage at the virus-host interface in the distal lung, and to defining pathways and mediators of organ regeneration in the context of viral infection, focusing on the interaction of macrophages with parenchymal cells of the distal lung and the epithelial stem cell niche.
Moreover, we study mechanisms that lead to increased susceptibility to bacterial infections during viral pneumonia or acid aspiration with a focus on alveolar macrophages. These aims will be achieved by using established models of in vivo virus infection, acid aspiration and bacterial superinfection of different levels of complexity (in vitro – ex vivo – in vivo) combined with analyses of patient samples, using FACS and cell sorting (LSR Fortezza, FACSAriaIII), NGS including single cell RNA-Seq, organoid modeling, and high-resolution microscopy/ life imaging techniques. The ultimate goal is to find novel disease biomarkers defining susceptibility to and recovery from ALI, and to identify distinct host targets to be harnessed for novel therapeutic strategies to combat severe respiratory viral infection, and bacterial superinfections due to viral or non-infectious insults in the lung.
Interdisciplinary collaboration in search of new therapeutic strategies to fight lung infectious diseases
Our Team
Our team at the chair consists of dedicated scientists and researchers with diverse backgrounds and expertise. Together, we strive to understand the origins and progression of respiratory diseases in order to develop new diagnostic and therapeutic approaches.
Our team leader, Professor Dr. Herold, is a renowned expert in the field of lung research. With extensive experience in the study of respiratory infections, she has published numerous scientific papers. Under her guidance, our team members are actively involved in various projects focused on understanding the molecular and cellular mechanisms of lung inflammation and other respiratory conditions.
We take pride in having talented young researchers and students as part of our team, benefiting from the experience and expertise of our seasoned researchers. Together, we are committed to advancing medical research and making groundbreaking discoveries in the field of respiratory diseases.


Funding & Cooperation Partners
Herold Lab is always open for collaborations with partners from academia, industry, and the public sector. We are interested in translating our research findings into practice and jointly developing innovative solutions. Funding is a crucial part of our work, enabling us to conduct our research at the highest level. Therefore, we appreciate any contribution that supports us in achieving our goals. Please feel free to contact us for more information.
Recent developments in our fields of expertise
For progress, sharing the latest medical knowledge is essential.
Our location
Department of Medicine V
Internal Medicine, Infectious Diseases and Infection Control
University Hospital Giessen und Marburg (UKGM)
























